Dr. Glenn Barnhart provides educational material for young surgeons and surgical trainees so that they may adopt successful techniques related to the On-X aortic and On-X mitral heart valves.
Please Note:
The views expressed during this presentation are the speaker’s own and do not necessarily reflect those of Artivion, the speaker’s employer, organization, committee or other group or individual. Unattributed data, device selection, and procedural guidance is a matter of physician preference are presented on the basis of the individual speaker’s observations and experiences and should be treated accordingly. Federal law restricts the devices discussed herein to sale by or on the order of a physician. Refer to the Instructions for Use and other product insert documentation that accompanies each of these devices for indications, contraindications, warnings, precautions, possible complications, and instructions for use.
On-X® Prosthetic Heart Valve – Instructions For Use
Products not available in all markets. The content of this presentation, including any copyrightable content included herein, is used with permission from the speaker. All products and indications are not available/approved in all markets. All trademarks are owned by Artivion, Inc. or its subsidiaries. On-X Life Technologies, Inc., Jotec GmbH, and Ascyrus Medical GmbH are wholly owned subsidiaries of Artivion, Inc. . © 2023 Artivion, Inc. All rights reserved.
Related Videos
Minimally Invasive Mitral Valve Replacement Using On-X® Mitral Heart Valve Cases
Dr. Mario Castillo-Sang provides educational material for young surgeons and surgical trainees so that they may adopt successful techniques related…
Surgical Technique for On-X® Aortic Heart Valve Implantation
Dr Glenn Barnhart provides educational material for young surgeons and surgical trainees so that they may adopt successful techniques related…
Surgical Technique for On-X® Mitral Heart Valve Implantation
Dr. Glenn Barnhart provides educational material for young surgeons and surgical trainees so that they may adopt successful techniques related…

On-X Mitral Valve Replacement: 5 Case Videos
Mario Castillo-Sang, MD, shares five cases of mitral valve replacement with On-X mechanical valves.
On-X Mitral Valve MV Replacement
Professor Roberto di Bartolomeo from University of Bologna, Italy performs a mitral valve replacement with leaflet preservation with On-X prosthetic…
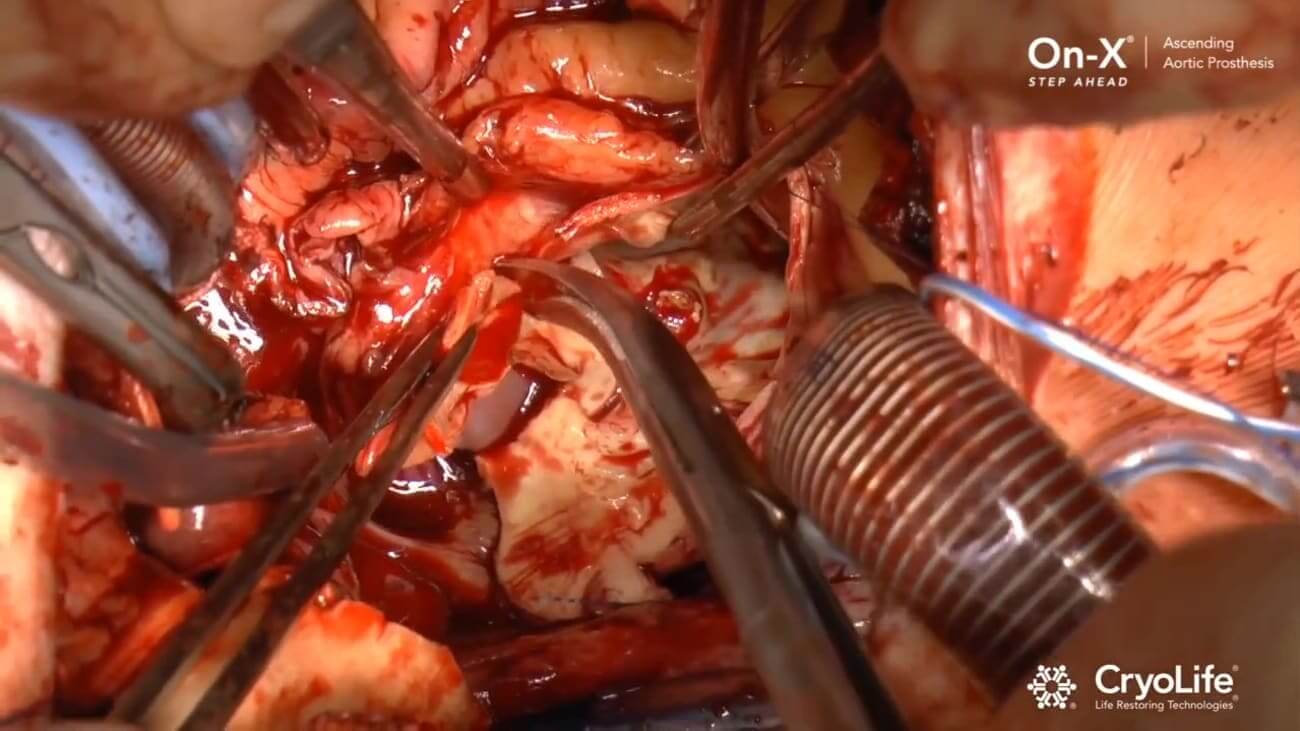
On-X AAP Implant Video
Minimally Invasive Aortic Root Replacement using an On-X Ascending Aortic Prosthesis with thanks to Prof. Malakh Shrestha of Hannover Hospital…
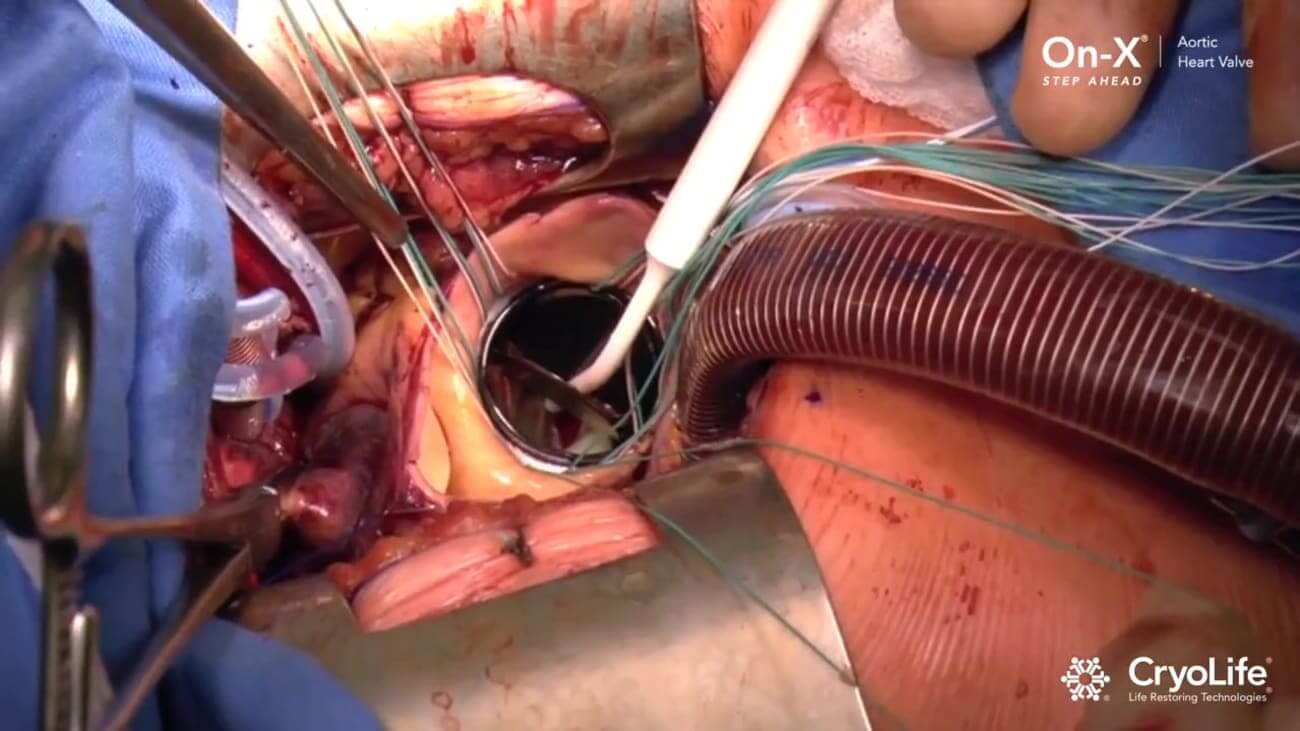
On-X Aortic Valve AVR via MIS Procedure
View a minimally invasive surgical (MIS) procedure of an aortic heart valve replacement using an On-X Aortic Valve featuring an…
